Nail Psoriasis Treatment
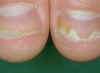
Nail psoriasis
Nail psoriasis treatment twice per day using Psoriasis-Ltd III can quickly and effectively improve both toenails and fingernails. Simply wet the affected toenails or fingernails, and glide the Psoriasis-Ltd III disk over the skin surrounding the toenail or fingernail as well as the entire nail psoriasis area itself. A small invisible amount of the Psoriasis-Ltd III ingredients will dissolve off onto the crevices around the fingernail or toe-nail, and the ingredients will penetrate fingernail or toenail. Likewise, make an application of Psoriasis-Ltd III with the fingers wet while the fingers and toes are pointing upward so that Psoriasis-Ltd III can easily penetrate under the nails. Nail Psoriasis can affect both the toenails and fingernails. Psoriasis of the fingernails and toenails is common but can be very difficult to treat. About 50 percent of persons with active psoriasis have psoriatic changes in fingernail and/or toenail. In some instances psoriasis may occur only in the nail and nowhere else on the body. Psoriatic changes in nails range from mild to severe, generally reflecting the extent of psoriatic involvement of the nail plate, nail matrix (tissue from which the nail grows), nail bed (tissue under the nail), and skin at the base of the nail. Damage to the nail bed by the pustular type of psoriasis can result in loss of the nail.
Symptoms of Nail Psoriasis
Pitting of the nail may be an early sign of nail psoriasis, although pitting can also occur in other diseases. Sometimes the nails develop a yellowish color and become thick. The nail may crumble easily and be surrounded by inflammation. Nail pitting looks as if a biro tip has pushed a dip into the nail and there may be up to 10 on each affected nail. Having pits in the nails does not mean that the psoriasis is going to behave any differently than if there are no nail pits present. No treatment is available for nail pitting and it is not usually necessary to treat this anyway. Nail pitting does NOT mean that other types of nail problems will arise.
Another possible symptom is detachment of the nail from the nail bed. During this process, the nail becomes whitish in appearance. Sometimes it becomes so badly damaged that it starts to crumble. Nail psoriasis can affect the connective tissue that forms the nails. Other signs of nail psoriasis include the appearance of dark spots resembling oil droplets on the nails, the build-up of flaky skin cells under the nails. Separation or loosening of the nails from their beds results in a condition known as Onycholysis. Onycholysis is when the nail bed develops a build up of keratin causing the nail to appear white when it is viewed from above. It usually starts from the end of the nail and works back. This may be the only sign of psoriasis and may affect only one finger or toenail alone and there may be no other skin rash of psoriasis. Onycholysis may affect only one fingernail and never become more extensive, but in some people it can affect more than one nail. There is no way of predicting this. The nail can lift off from the nail bed and the nail can sometimes be lost. It may or may not grow back normally.
Occasionally the build up of keratin beneath the nails in psoriasis can be very marked and lead to the affected nail becoming thickened and raised. When this happens it is called Onychodystrophy. This can be sore and painful and some sufferers may also find the appearance embarrassing due to comments made by others. The other diagnosis could be a fungal infection of the nail in which case clippings of the crumbly keratin beneath the nail should be sent for culture. Sometimes it can be difficult to tell between the two.
Psoriasis of the nails can resemble other conditions such as chronic infection or inflammation of the nail bed or nail fold. Psoriasis of the toenails can resemble chronic fungal infection of the nails. About one-third of people with nail psoriasis may have a fungal infection, which, if treated, could help their nails to improve. Some treatments used for skin psoriasis also may improve the condition of the nails.
Treatment
If your nails are affected by psoriasis, try the following:
- Trim your nails to reduce the risk of injuring them; trauma can worsen nail psoriasis.
- Try soaking affected nails and follow up with moisturizer. Carefully file thickened toenails with an emery board after soaking.
- Reduce toenail pressure and friction - which can cause toenails to thicken -- by wearing well-fitted, roomy shoes.
- Consider using nail hardeners or artificial nails that can help to improve the appearance of intact nails.
- Talk to your physician if deformed nails are a problem for you. They may be surgically removed and replaced with artificial nails.
A person with psoriatic nails should avoid any injury-bumps, scrapes, etc.-that may trigger a worsening of psoriasis, which is a condition called Koebner's phenomenon. Skin injury. Injury or trauma can make psoriasis worse. Patches of thick, flaky skin may appear following a burn, graze, or rash. If someone is prone to outbreaks of psoriasis, it is important to promptly treat rashes such as those caused by allergies to medication. Otherwise, the rash could lead to a flare-up of psoriasis. The Koebner phenomenon occurs in about 1 in every 4 people with psoriasis. Nail psoriasis is treated by the dermatologist as part of the overall treatment of the disease.
Nail psoriasis is frequently associated with psoriatic arthritis. Certain medications may make psoriasis worse. These include lithium (prescribed to treat bipolar disorder, beta blockers (prescribed for heart problems), anti-malarial drugs, and nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen are available by prescription or over the counter for pain relief. NSAIDs are often used to treat psoriatic arthritis. In such cases, the benefits and risks of treatment need to be carefully assessed. Flare-ups of psoriasis caused by NSAIDs usually respond to treatment.

